Can Heartworm-Positive Dogs Safely Have Surgery? A 2026 Study Says Bleeding Risk Is Unchanged
A new May 2026 study finds that heartworm-positive dogs do not bleed more than healthy dogs during routine surgery — but cardiac and thromboembolic risks still matter. Here's the full picture.

Quick Summary
A new May 2026 study published in Frontiers in Veterinary Science looked at whether dogs with heartworm disease bleed more during routine surgery. The reassuring answer: primary surgical bleeding and platelet function were unchanged in heartworm-positive dogs compared to healthy controls. For pet parents weighing surgery while a dog is still in treatment, this is meaningful, evidence-based good news — but it doesn't change the urgency of treating heartworm itself.
If your dog has tested positive for heartworm and also needs a procedure — a dental, a mass removal, a spay or neuter — your veterinarian's first instinct has historically been caution. Heartworm disease is a vascular disease. The worms live in the pulmonary arteries and right side of the heart, and chronic infection causes inflammation, endothelial damage, and changes to the way blood flows and clots. It made intuitive sense that bleeding might be worse. A new 2026 study finally tested that assumption with modern hemostasis tools — and the results may change how vets counsel owners.
Below is what the study found, what it does not say, and how it fits into the broader picture of heartworm care in 2026. We'll also link out to related Dog Health & Wellness coverage on our blog so you can see the full surveillance and prevention picture.
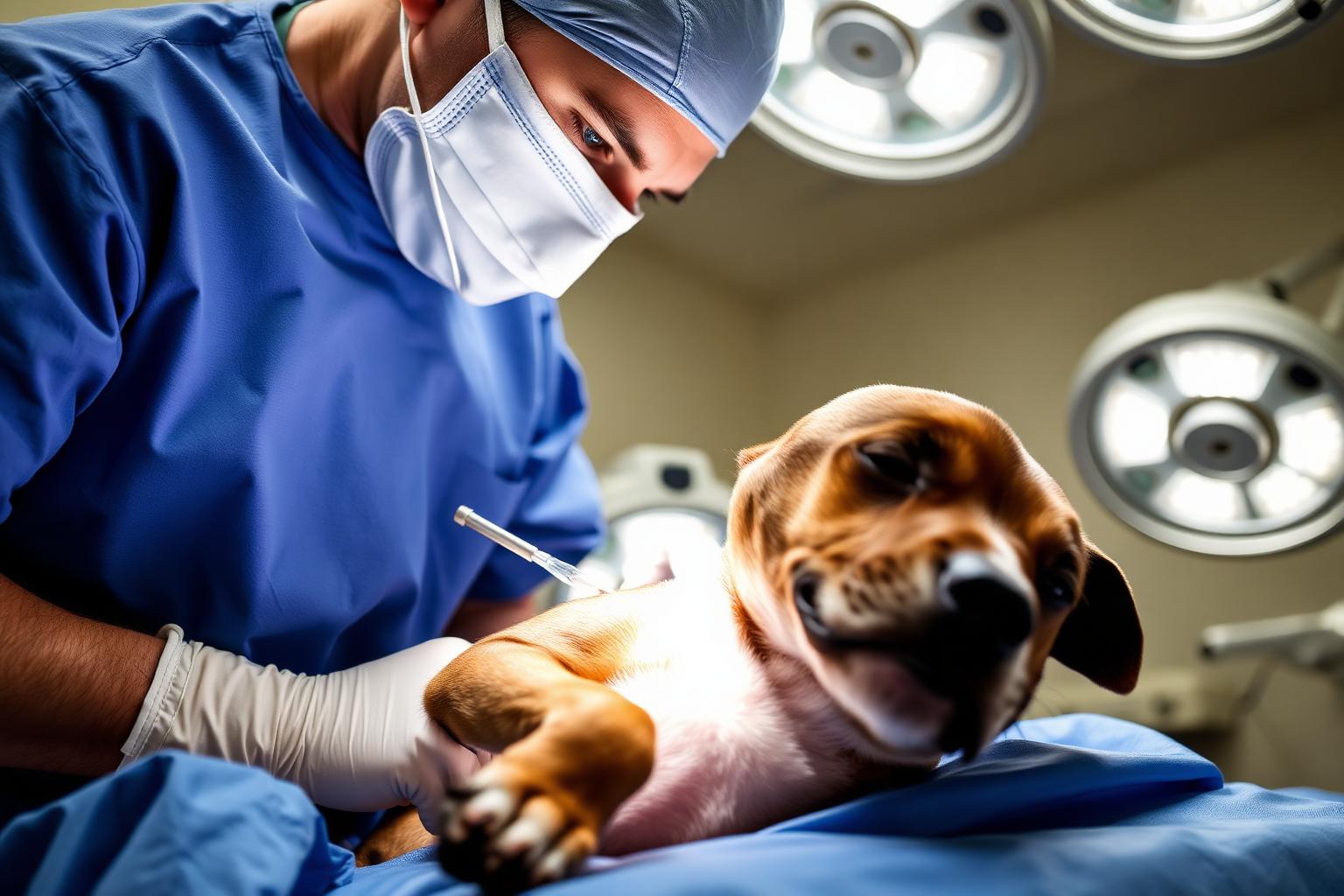
What the 2026 study actually measured
The paper, "Primary surgical bleeding and platelet function are unchanged in heartworm-infected dogs," was published in Frontiers in Veterinary Science on 7 May 2026. Researchers compared dogs naturally infected with Dirofilaria immitis to a healthy control group, then looked at three things that matter when a dog goes under the knife:
- Primary surgical bleeding — how much a small standardized incision actually bled during a controlled surgical model.
- Platelet function — measured with modern point-of-care platelet aggregation testing, not just a platelet count.
- Standard coagulation panels — PT, aPTT and fibrinogen, the same tests your own vet runs before sedation.
Across all three buckets, the heartworm-positive dogs were statistically indistinguishable from the healthy dogs. Bleeding times were comparable. Platelets aggregated normally in response to standard agonists. Clotting times were within reference intervals.
Why this matters for routine procedures
For decades, "heartworm positive" has been treated as a near-automatic flag to delay elective surgery — including dentals, lump removals and even spay/neuter — until after the dog completed adulticide treatment and the mandatory exercise restriction period. That can mean six to nine months of waiting. The 2026 data suggest that, at least for primary surgical bleeding, the worry was overstated for clinically stable dogs without overt cardiac disease.
Veterinary Disclaimer
This article summarizes a single 2026 study and is not medical advice. Heartworm disease still carries real anesthetic, cardiac and thromboembolic risks. Always discuss your specific dog's stage, echocardiogram findings and bloodwork with your veterinarian before scheduling any procedure.
What this study does NOT say
This is the part owners can easily misread. The headline is "bleeding is unchanged" — but that's a narrow finding. It does not mean heartworm-positive dogs are at the same overall surgical risk as healthy dogs. Here's what's still true:
1. Anesthetic risk is still elevated
Dogs with pulmonary hypertension, right-sided heart enlargement or significant pulmonary artery damage are still riskier under general anesthesia. The bleeding-time finding doesn't change cardiac reserve. A pre-anesthetic echocardiogram remains the gold standard for staging.
2. Pulmonary thromboembolism risk persists
The biggest peri-treatment killer in heartworm disease is dead-worm thromboembolism after melarsomine injections. Surgery during or immediately after adulticide treatment can compound that risk. The 2026 study deliberately measured primary surgical bleeding — it did not address clot showering from the pulmonary arteries.
3. Severe (Class 3–4) cases were under-represented
Like most hemostasis studies, the cohort skewed toward clinically stable, mildly-to-moderately affected dogs. Dogs in caval syndrome, with severe right-heart failure, or with overt DIC were not the population studied. Those dogs absolutely can have abnormal hemostasis.
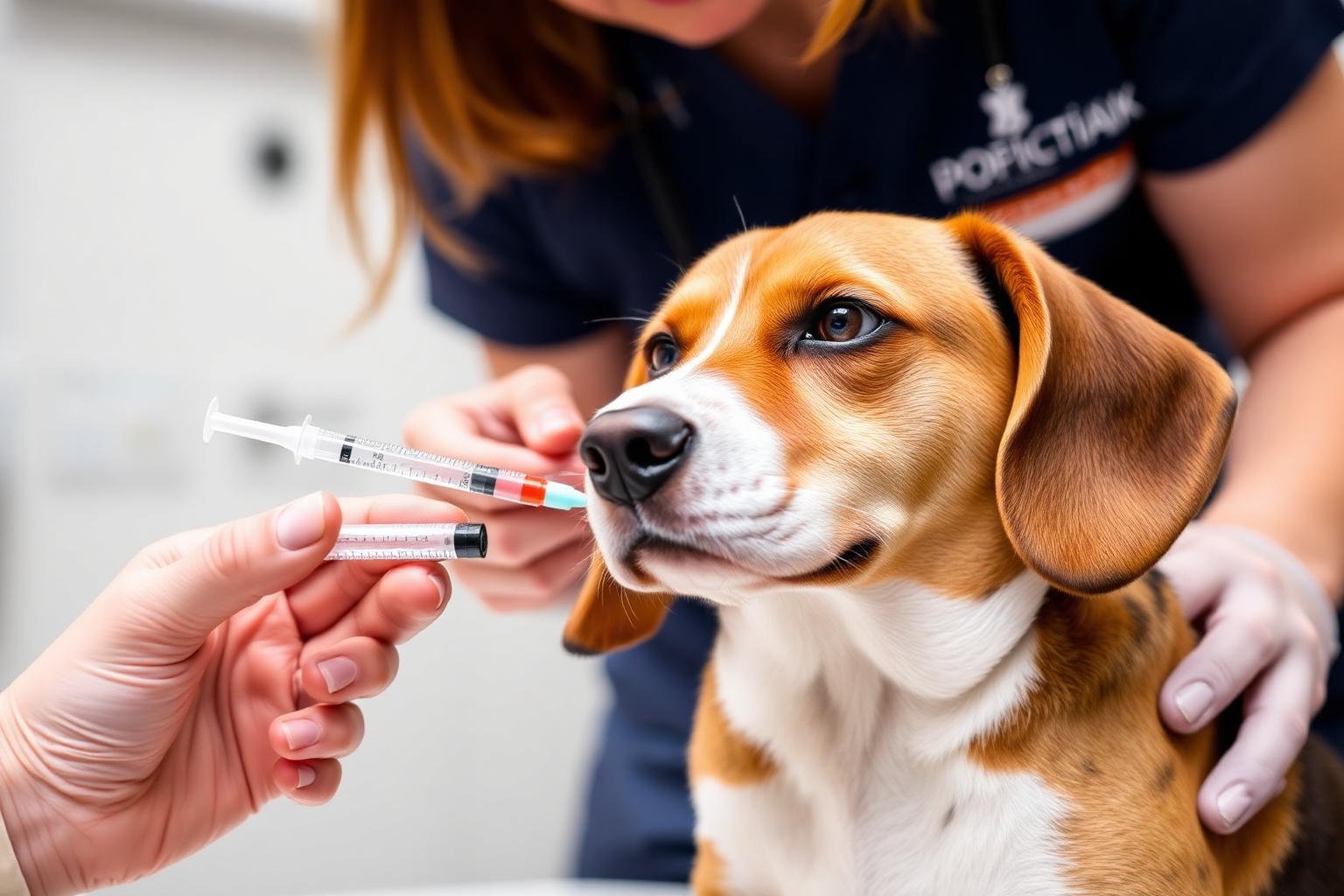
How heartworm actually affects the body
To understand why this finding is notable, it helps to picture what's happening inside an infected dog. Adult D. immitis worms — sometimes a foot long — live in the pulmonary arteries. Their presence triggers chronic inflammation of the artery walls (endarteritis), thickening, and turbulent blood flow. Over months to years, this can lead to:
- Pulmonary hypertension
- Right-sided heart enlargement and eventually right-sided heart failure
- Glomerular kidney damage from circulating immune complexes
- In severe cases (caval syndrome), worms physically blocking the tricuspid valve
Older small studies had hinted at platelet activation and consumption in heavily infected dogs — which is why the bleeding question was open in the first place. The 2026 paper's contribution is showing that, for the average naturally-infected dog walking into a clinic, those subclinical changes don't translate into measurable bleeding at the scalpel.
Practical takeaways for owners in 2026
If your dog just tested positive
Don't panic about needing to cancel an upcoming dental or lump removal on bleeding grounds alone. Have a frank conversation with your vet about cardiac staging instead. Ask: "What does her chest X-ray and echo look like? Is she Class 1, 2, 3 or 4?" The answer matters far more than the bleeding question.
If your dog is mid-treatment with melarsomine
Strict exercise restriction for the full recommended period (typically 6–8 weeks after the final injection) is still non-negotiable. Elective surgery during this window is still discouraged because of thromboembolism risk, not bleeding risk.
If your dog is on year-round prevention
Keep going. Annual testing is still recommended even on prevention, because no preventive is 100%. For more on what's changing in canine wellness research this year, see our coverage of the 2026 Italian study on second cancers in dogs and the Texas A&M ractopamine cardiac study — both reinforce the value of structured surveillance.
If you have a senior dog facing surgery
Heartworm status is one variable. Cognitive and metabolic status are others. Our piece on why large-breed brains age slower than their bodies is a useful companion read for owners of older dogs heading into anesthesia.
Key Takeaways
- The May 2026 Frontiers in Veterinary Science study found no measurable difference in primary surgical bleeding or platelet function between heartworm-positive dogs and healthy controls.
- This does not mean heartworm-positive dogs are anesthetically equivalent to healthy dogs — cardiac and thromboembolic risks remain.
- Cardiac staging (chest X-rays, echocardiogram) matters more than bleeding tests when deciding whether to operate.
- Severe (Class 3–4) cases were under-represented and should still be approached with extra caution.
- Year-round prevention plus annual testing remains the simplest, cheapest line of defense.
Frequently Asked Questions
Can my heartworm-positive dog safely have a dental cleaning?
Often yes, if the dog is clinically stable and not currently mid-adulticide treatment. The 2026 study supports the idea that bleeding control will be normal. Cardiac stability is the bigger question — ask your vet about a pre-anesthetic echo.
Should I delay my dog's spay or neuter because of heartworm?
Many vets prefer to treat heartworm first because of the long exercise-restriction window. The new bleeding data may shift that calculus for stable dogs, but it's still a case-by-case call.
Does this study apply to dogs in caval syndrome?
No. Severely affected dogs were not the study population, and caval syndrome is a surgical emergency with very different hemostatic risks.
What about dogs on aspirin or other anti-platelet drugs as part of heartworm care?
The study measured untreated dogs versus controls. If your dog is on aspirin, clopidogrel or NSAIDs, those drugs independently affect platelet function and the conclusions don't transfer cleanly.
How often should I test even if my dog is on prevention?
Annually, per the American Heartworm Society. Missed doses, vomiting after a dose, or rare resistant strains can all let infection slip through.
Frequently Asked Questions
Can my heartworm-positive dog safely have a dental cleaning?+
Often yes, if the dog is clinically stable and not currently mid-adulticide. The 2026 study supports normal bleeding control; cardiac stability is the bigger question.
Should I delay my dog's spay or neuter because of heartworm?+
Many vets still prefer to treat heartworm first because of the long exercise-restriction window, but the new bleeding data may shift that for stable dogs.
Does this study apply to dogs in caval syndrome?+
No — severely affected dogs were not the study population.
What if my dog is on aspirin or NSAIDs?+
Those drugs independently affect platelet function and the conclusions don't transfer cleanly.
How often should I test even if my dog is on prevention?+
Annually, per the American Heartworm Society.
Sources
Related Reading
Liked this story?
Share it with someone who should read it.
More from Dog Health & Wellness

Ractopamine and Your Dog's Heart: What the 2026 Texas A&M Study Means

Sports, Walks and a Sharper Senior Dog: What the 2026 ELTE Study Reveals About Canine Dementia
